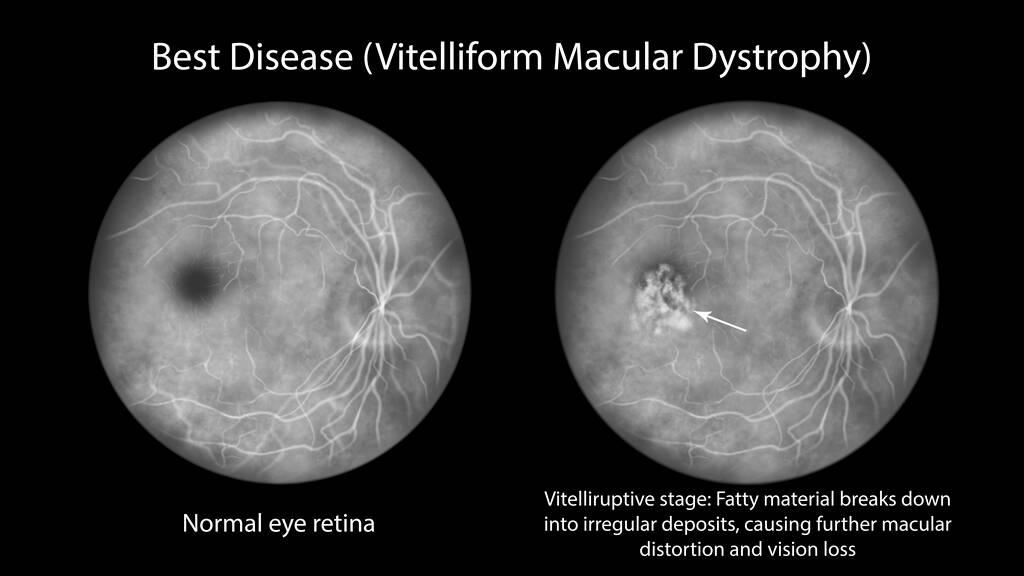
Diabetic Retinopathy Is An Eye Condition That Affects Eye Retina
Diabetic Retinopathy is an eye condition that affects the retina and is a complication of diabetes. It occurs when high blood sugar levels cause damage to the small blood vessels in the back of the eye, leading to vision problems and even blindness if left untreated. This condition can occur both in those who have been diagnosed with Type 1 or Type 2 diabetes, as well as in individuals with pre-diabetes. Early detection and treatment of diabetic retinopathy are important for preventing further damage to vision.
Definition of Diabetic Retinopathy
Diabetic retinopathy is a condition caused by damage to the small blood vessels in the retina, the light-sensitive tissue at the back of your eye. This damage can cause vision problems such as blurred vision, dark spots, or complete loss of sight. It’s one of the most common complications associated with diabetes and can lead to permanent blindness if left untreated.
Diabetic retinopathy is caused by high blood sugar levels over an extended period of time that damage small blood vessels in your eyes. Over time, these damaged vessels become swollen and leak fluid into your retina causing it to swell and distort your vision. In more severe cases, new abnormal blood vessels may grow on the surface of your retina leading to bleeding that further damages your vision. Diabetic retinopathy in Singapore is a sensitive eye condition that often leads to eye surgery.
Early signs of diabetic retinopathy include blurred or distorted vision due to swelling or leaking fluid from damaged blood vessels in the eye. As it progresses you may start seeing floaters or flashes in front of you when there are no lights around you – this could indicate bleeding within your eye from growing abnormal new blood vessels on its surface. If left untreated, diabetic retinopathy can cause permanent blindness as well as other serious complications such as glaucoma and cataracts which require surgery for treatment if caught.
Causes of Diabetic Retinopathy
Diabetic retinopathy is a serious eye condition that can lead to permanent vision loss and blindness. It affects people with diabetes and is the leading cause of blindness in adult Americans aged 20-74.
Diabetic retinopathy occurs when high blood glucose levels damage the tiny blood vessels in the back of the eye (retina). The retina is responsible for processing images and sending them to the brain for interpretation. When these vessels become damaged, fluid can leak out into surrounding tissue, causing swelling and blurred vision. Over time, new abnormal vessels may form on the surface of the retina leading to bleeding within or outside of the eye and resulting in further vision loss.
There are two main causes of diabetic retinopathy: poor control of blood sugar levels over long periods of time and elevated levels of lipids (fats) in your bloodstream.
When it comes to poorly managed diabetes, high blood sugar levels over a long period cause damage to small capillaries that supply oxygenated blood to your eyes’ retinas resulting in impaired vision or even complete blindness if not treated early enough.
Symptoms of Diabetic Retinopathy
Diabetic retinopathy is a common complication of diabetes and one of the leading causes of blindness. It occurs when high blood sugar damages the blood vessels in your retina, which is the light-sensitive tissue at the back of your eye. Fortunately, early detection and treatment can help slow or prevent vision loss. Knowing what to look for can help you recognize the symptoms of diabetic retinopathy before it becomes severe.
Eye Retina
The first symptom to be aware of is blurred vision. As small blood vessels become damaged from too much sugar in your bloodstream, they leak into the retina causing it to swell and blur your vision. This can happen suddenly or over time, so if you notice changes in your vision it’s important to have an eye exam right away.
Another symptom is dark spots or floaters that appear as specks or strings drifting through your field of view. These are caused by bleeding inside the eyeball due to weakened blood vessels that can no longer hold back fluid from leaking out into other parts of the eye.
Diagnosing and Treating Diabetic Retinopathy
Diabetic retinopathy is a potentially blinding eye disease, caused by diabetes. It affects the retina, which is the light-sensitive tissue at the back of the eye. As blood vessels in the retina become damaged, they can leak fluid and cause swelling (edema) or abnormal new blood vessels may form (proliferative retinopathy). Both types of diabetic retinopathy can cause vision loss if not treated promptly.
The first step in diagnosing diabetic retinopathy is a comprehensive dilated eye exam which should be done annually for people with diabetes or those at risk for developing diabetes. During this exam, an ophthalmologist will use special magnifying lenses to examine your eyes and look for signs of damage including leaking blood vessels and swelling. Your doctor may also take photos of your retina to track any changes that occur over time.
Treatment options depend on how advanced your condition is but often include laser surgery or injections into the eyeball with medications that help reduce inflammation and abnormal blood vessel growth. Laser surgery works by targeting abnormal blood vessels and sealing them off to prevent further leakage while injections help reduce swelling and stop new vessel formation from occurring.
Prevention of Diabetic Retinopathy
Diabetic retinopathy is a serious eye condition that affects people with diabetes. It can cause vision loss and even blindness if left untreated. Fortunately, it is also one of the most preventable forms of eye disease. By following simple lifestyle changes, people with diabetes can reduce their risk of developing diabetic retinopathy and maintain healthy eyesight.
The first step in preventing diabetic retinopathy is to keep your blood sugar levels under control. High blood sugar levels over time can lead to damage to the delicate blood vessels in the retina of your eyes, resulting in diabetic retinopathy. The American Diabetes Association recommends self-monitoring your blood glucose level at least four times a day and keeping it within normal limits as much as possible. Additionally, eating a balanced diet high in fibre and low in refined carbohydrates will help you keep your glucose levels steady throughout the day.
It’s also important for people with diabetes to have regular comprehensive dilated eye exams from an ophthalmologist or optometrist at least once a year (or more often if recommended by their healthcare provider).
Conclusion
In conclusion, diabetic retinopathy is a serious eye condition that can lead to vision loss and blindness if left untreated. Early detection and prompt treatment are key to reducing the risk of permanent vision damage. It is important for people living with diabetes to have regular eye exams to monitor for signs of this condition. With careful management, those at risk can reduce their chances of developing vision complications associated with diabetic retinopathy.





